 To our little Eva, with whom we lived 14 unforgettable months:
To our little Eva, with whom we lived 14 unforgettable months:
Eva left abruptly on February 10th, 2019 at the age of 14 months.
We became informed about the genetic mutation ASXL 1, and the BO Syndrome, at the end of July 2019. This is why we would like to give our testimony today, and to do so more specifically with regards to the care for our daughter.
Please read Eva’s story in the original text (French) below.
Eva was born in Lyon, France on December 1st, 2017, one week before her due date, in a private maternity clinic.
She is our first child. As such, we had decided to keep the baby’s sex a surprise and were more than ecstatic when we found out that she was a wonderful little girl.
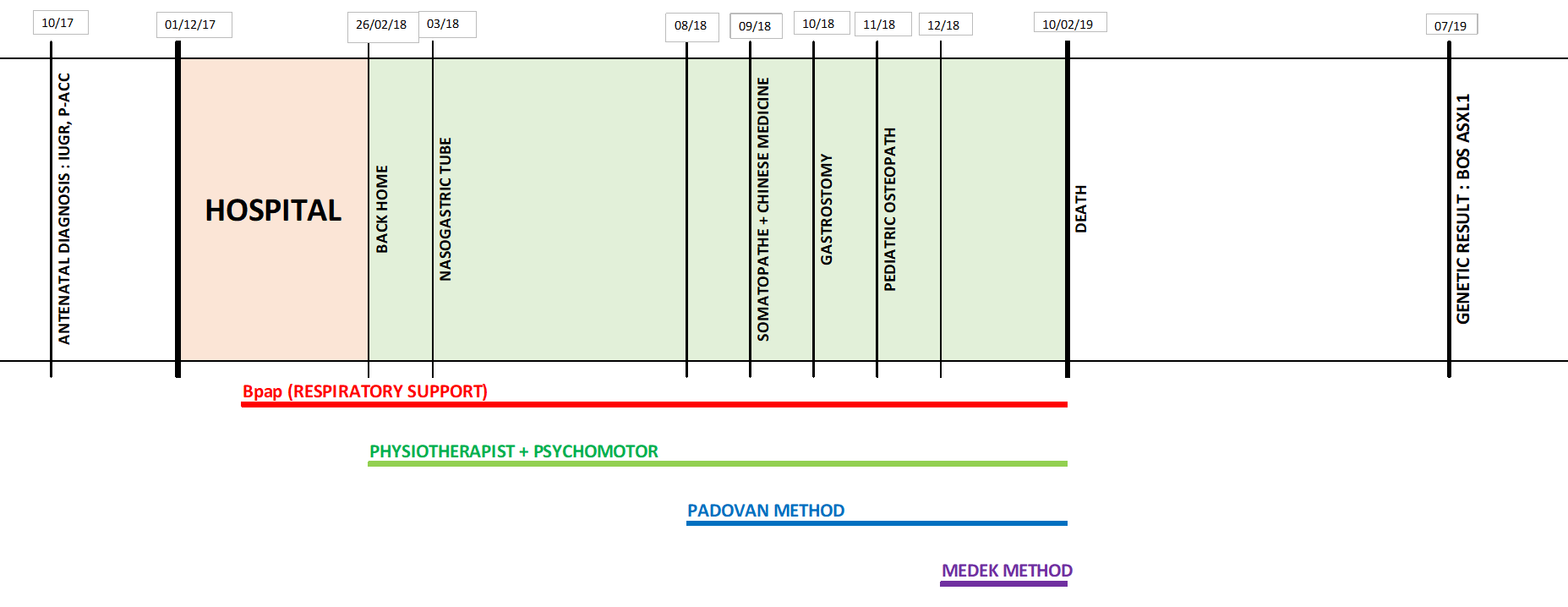
The pregnancy went well, with the usual monthly check-up appointments. The doctors discovered a delay of in-utero growth and a partial agenesis of the corpus callosum at 7 and half month of the pregnancy. Despite many in-depth tests and exams, no other abnormality was detected. Therefore, we remained confident!
The delivery was performed by C-section under full anesthesia after the doctors detected fetal cardiac distress. Eva had also changed her position in-utero to a breech position the day before delivery.
The doctors had a lot of difficulty to remove Eva from the womb. As a consequence, Eva received a lot of anesthetics (through mom’s receiving it). Later, the physicians considered that factor to be the cause of all of her subsequent ailments.

At birth, Eva weighed 2,550 kg for 45cm length.
As far as physical characteristics go, Eva was rather thin, with a short neck. She had an abundance of black hair and some birth marks on her eyelids. She had a small cleft palate as well as a frenulum of tongue (which was cut when she was 2 months old).
Doctors readily noticed her hypotonia as well as her hands and wrists being turned inward and hypertonic.
She was immediately placed in the NICU because her eyes rolled back and her oxygen levels irregular.
She was put on an oxygen regimen for 4 days, after which she had improved and seemed well recovered. Consequently, she was only monitored for her oxygen levels and cardiac rhythm,
Eva was subject to bradycardic episodes while bottle feeding, something that she however enjoyed very much doing in the beginning. She had some difficulty coordinating sucking and swallowing.

One week after her birth, she stayed in the hospital room with us while remaining under constant monitoring. This arrangement allowed us to take care of our little girl full-time while benefitting from the presence and help of nurses and doctors who could intervene at a moment’s notice.
An oesophagus-gastric reflux (OGR) was detected when she was 1 week old because of her cough and weak voice. However, Eva did not vomit. Doctors gave her a treatment for her reflux (Inexum). This was the only medicine Eva ever took, but she took it all her life.
After 3 weeks, Eva had more frequent bradycardic episodes while bottle-feeding, and with those came more frequent oxygen desaturation episodes.
At that juncture, the doctors considered that there might be a more serious problem not in link with the delivery.
We then stopped bottle-feeding Eva. A naso-gastric tube was placed in order to relieve her.
At one month old, Eva was transferred to a specialized pediatric hospital nearby our home with renowned specialists, in order for her to undergo further and more in-depth tests.
Immediately, we were brought under the care of a pediatric neurologist and a pediatric pulmonologist who informed us of their diagnostic: Eva had severe sleep apnea (due to tracheomalacia–or soft windpipes, and a problem of command at the brainstem), axial hypotonia and peripheral hypertonia (tense arms, wrists and hands), as well as a severe developmental delay (Eva had poor eye contact, no responsive smiling, and very little interaction). However, the doctors had no idea about what caused those ailments. The only visible abnormality was the agenesis of the corpus callosum, but that alone did not explain all the problems.

Her cerebellum and kidneys were smaller, but at her 1-year old exams, both the kidneys and cerebellum were of a normal size for her size.
With regards to her apnea episodes, she was given respiratory assistance via BpaP (air only, no oxygen) to be used 18 hours per day. She also needed to have her oxygen levels and cardiac rhythm constantly monitored by scope (oximetry).
Once her breathing was stable, Eva was able to resume bottle-feeding.
The doctors estimated however that despite her weight gain, it remained insufficient given her low weight at birth. They put her on a regimen of highly enriched milk (but hard to digest). It is at that moment that Eva started to vomit regularly, 2-3 times a day (she was 2 months old).
Once her condition became fully stable, and we were trained for her care, Eva was able to leave the hospital, and we finally could take her home with us (Eva was then almost 3-months old).

We, the parents, both made the choice to reduce our work time to only half-time, so that we could take turns and be available to care for our daughter full-time ! This was the best decision we ever made!
The return home was complicated in relation to feeding : Eva was eating less and less. We therefore had to once again insert a nasogastric tube a few weeks after our return.
However, the tube was used in the beginning (for 1 month and a half) only at night, with the purpose to make it easier on us, so we only had to feed her during the daytime. With us, Eva was constantly alternating her feedings between full bottle-feeding and partial bottle-feeding, and we could never figure out why she would feed well on some days and not on others.
She continued to take her reflux medication and her vomiting fluctuated (she vomited small quantities)…She often was chewing, as if chewing gum, but that was due to her reflux.
Night-times were complicated during the first 2 months at home.
Generally speaking, Eva was a baby that cried very little, and we do not know whether that was due to lack of pain/discomfort, or simply because she expressed pain differently, but the doctors would not say anything about it. Eva woke up often, cried rarely, had muscle tension and twisted her little body. We could tell that she was uncomfortable, and it was hard for us to witness it.
Consequently, we made the decision to change her milk (to lactose-free and cow protein free milk, which is easier to digest, even though Eva could tolerate cow milk) and to stop feeding her at night time in order to only feed her during daytime on a scheduled basis. Within a few days, Eva was doing better. It was a relief for us to see her sleep serenely.
Simultaneously, her pediatrician had noticed that Eva started to develop a scoliosis on her left side that she deemed barely correctable. (Despite all the follow-ups and exercises set up for her, we never managed to reduce or fully correct the scoliosis)
After our return home, Eva received the help of many therapists : physical therapy twice a week and psycho-motricity therapy once a week in order to catch up with her fine motricity delay. She also saw a speech pathologist twice a month for her oral problems (doctors thought that her feeding difficulties were due to some orality abnormalities)

Eva was making slow but steady progress. At 6 months, she started to hold her head up well, she was able to lock her eyes on objects and people, and to follow their movements. But as far as her motor skills, she had only progressed a little bit (her arms, hands and wrists were very tense, and we had the impression that it was painful).

Eva was very often in our arms, and she kept her hands wrapped around our fingers, certainly a means for her to be reassured (and for us, a sweet time of sharing), but that also helped her not clench her fists too tight (hypertonia).

On the other hand, her scoliosis continued to worsen.
We therefore looked for other efficient and additional help methods.
The first method we discovered is called PADOVAN, a method of neurofunctional psychomotor reorganization (created in Brazil). Therapists that practice this method are still too rare, but we were able to start sessions for Eva when she was 8 months old; and that, twice a week.
We also consulted a doctor who practiced Chinese medicine when Eva was 9 months old (2 sessions followed by exercises to practice at home for 1 month).

We sought this with a view to help her relax, especially her arms, because we feared that her muscle tensions were painful for her, especially when we observed her tense little face…
Eva’s progress was impressive ! Within 2 or 3 months only, Eva held her head well, her arms, hands and wrists were relaxed and she started to use them.
Simultaneously, we noticed great progress in relation to her apnea. From her 8th month, Eva needed her breathing assistance only at night time and no more during the day!
We continued to monitor her as soon as she fell asleep though, even when she was not on respiratory assistance, so that we could monitor her oxygen levels and heart rhythm always.
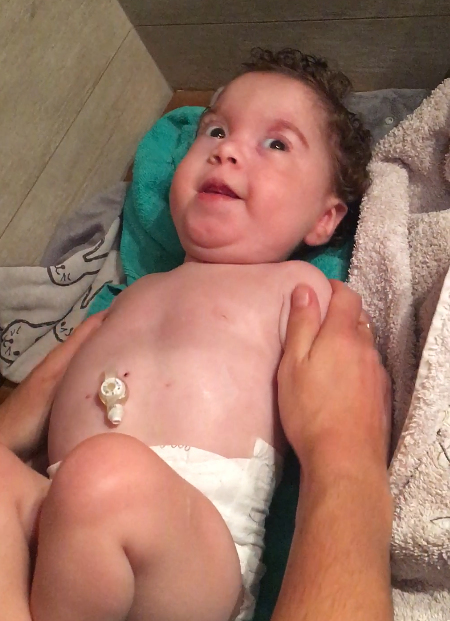
With regards to her feeding, that was always irregular. Also, Eva became able to pull out her gastric tube. When she was 10 months old, she underwent surgery to place a gastrostomy tube. It was a true relief for us as well as definite safety for the future!
Right away, the face of our little Eva changed : it became so much more relaxed!
During the months that followed the surgery, Eva continued to alternate between partial and total bottle feeding. She also was spoon-fed, but only a very small quantity at a time.
When Eva was 1-year old, she was able to start a new reeducation method (on top of the one she was already following) : the MEDEK method (developed in Canada, practiced by occupational therapists, but rarely practiced in France, where we live). This method consists of daily 15 minutes-long motor skills exercises, performed by the parents who are trained to do them. Eva improved tremendously!! In one month, she understood how she could stand up (of course, we were holding her)!

We also did 2 sessions with an osteopath specialized in pediatric care, this, still with the goal to relieve her of possible physical suffering.
All those methods were truly of great help. Eva made a lot of progress, and she loved doing the exercises. This is when she started to giggle and have laughing fits! Those became unforgettable moments !
Moreover, we the parents, together with the whole family, were actors of her progress, and made her do her exercises, and we took great pleasure to do so with our little sweetie girl.
We became very confident in what the future held, because apart from lingering feeding problems (bottle feeding was still irregularly successful and the vomiting occurred daily), Eva was making wonderful progress. Interaction was more and more frequent, especially during the last few weeks. She understood when we called her name.
During short periods, Eva had some sleep difficulties (mostly when she suffered digestive discomfort), but generally speaking, she slept well during the night, between 10 and 11 hours, and only woke briefly, no more that twice per night.
Eva was growing well (2 cm per month), but weight gain was still a problem: at 14 months, she weighed 7 kg for 70 cm, and the circumference of her skull was 43cm.
We always took Eva everywhere with us (taking along all the machines she needed did not bother us at all), We went on hikes, to friends’ houses, in public places, at family gatherings and even on vacation (we flew abroad at Christmas 2018).

Eva was never sick during her 14 months of life, never had an infection. Even the doctors were surprised at that fact (they did not know her syndrome then). For us, Eva had a great immune system.
In our eyes, Eva was a small baby like many others, who only was taking a little more time than others to develop.
As soon as she could leave the hospital, at almost 3 months old, Eva discovered the outside world, and her passion for contemplating trees started right away! She also adored looking at lights and colors.
She loved being cuddled, kissed, and cared for. Everyone took so much pleasure in being with her, taking care of our little angel.
Unfortunately, our whole life crumbled on February 10, 2019.
We had left Eva for the first time ever for her whole weekend with her grandparents, without us around (by that time, they knew very well how to take care of their grand daughter).
24 hours before her death, Eva got diarrhea, but we discounted it as a side effect to teething which had been apparent for a few days. On their way back from the weekend, while in the car with her grandparents, Eva lost consciousness. The first responders arrived on scene, at a rest area off the freeway, where they tried to revive her for 45 minutes, which proved of no avail. We, the parents, arrived at the scene too late. Our little girl was gone…
After several months of analysis, doctors discovered the presence in her organism of a Rotavirus, a serious gastroenteritis virus that causes severe dehydration and fever, but Eva only had a mild case of both.
The doctors concluded that her body and her brain were not able to react properly to the attack of the virus (it was the first time that Eva fell sick). This caused her blood flow to slow down and with it, her oxygen levels to drop. Her heart gave out first, leading to her loss of consciousness…this could all have coincided with the cardiac problems linked to the syndrome, despite the fact that Eva had not had any bradycardia for a long while (none that the monitor detected).
Since we have known what syndrome our little angel was affected with, we have been even more admirative and proud of Eva, and of her fight.
But we do not understand why our children must experience this.
We are sure of one thing : Eva has transformed us forever and has filled us with love, not only us the parents, but also all those around her. She positively changed our vision of life and of the afterlife, forever.
Thank you Eva for being here…
– by Marine Ercolani (Eva’s mom) and Romuald Boutin (Eva’s dad)

Thanks a lot for sharing Eva’s story.. a great help in taking care of my patients.
Best regards from Budapest
LikeLiked by 1 person
Many “normal” children don’t have such full lives in their first 10 years that you have given to your Eva. You really made her life full and gave her many experiences and adventures. I admire you for all of the healings you gave her, including Chinese Medicine. I hope you find peace in knowing this and that Eva lived for the time she was here, a life that exposed her to so many things in a short time.
LikeLiked by 1 person
je pense personnellement avec mon intime conviction qu’Éva s ‘ est incarnée sur notre terre afin de faire avancer la science, et en ce sens je la remercie pour tous les enfants a venir .
LikeLiked by 1 person
je n’en reviens pas de la volonté des parents et de leur dévouement pour la petite Eva .ils m’ont subjuguer dans leur détermination . de tous les sacrifices consentis.
je vous embrasse de du plus profond de mon être.
un grand père spolié de sa petite fille par la vie .
je vous aime .
LikeLiked by 1 person
Trop triste ma petite Eva partie si vite.
Je pense fort a tes parents. Repose en paix petit ange .
LikeLiked by 1 person
Je n’étais pas “pré-câblée” pour devenir grand-mère : les enfants ce n’est pas mon univers de vie, rien à leur dire… Mais Eva, là, ce fut autre chose : l’aimer à distance (1h par semaine pendant 3 mois), lui distribuer des tas de bisous, la promener partout (en poussette, en voiture, en avion, … dans les bras …), la nourrir, la brancher, veiller au bon fonctionnement de ses appareils, faire attention de ne pas arracher sonde ou câbles en se prenant les pieds dedans …etc Une vigilance de tous les instants mais toujours la récompense : elle ne pleurait pas, toujours calme, et ses joues qui appelaient les bisous, et ses bouclettes surgies d’on ne sait où. Lorsque les exercices Padovan déclenchaient tes fous-rires, c’était mon cadeau musical pour la semaine ! Je savais ton retard de développement mental et physique, mais quelle importance ? Depuis ton décès, dans le siège auto à côté de moi, j’ai apprivoisé l’idée de la mort, appris les gestes de 1er secours, découvert l’incroyable énergie déployée par le monde médical pour faciliter ton développement et comprendre tes difficultés, enquêté sur ‘la vie après la vie’, posé un regard nouveau sur la Vie. La naissance d’Eva, sa vie ponctuée de tous ses soubresauts, son décès, tout fut un enrichissement et un bonheur profond, sans questionnement sur le handicap, puisqu’accepté. Notre famille déjà soudée (et les amis) s’est encore plus solidarisée autour d’Eva, elle était le noyau de notre molécule et moi un des petits électrons attentifs et admiratifs (même si parfois ses difficultés à manger agaçaient cela ne durait pas). Merci pitchounette pour tout cela, tu n’es plus là ‘en vrai’ mais tu es là, autour, partout, tout le temps, avec tes ‘signes’ (les arbres, la couleur rouge, les conférences médicales ou philosophiques, ce site BOS, les milliers de photos et vidéos, …). La tristesse a disparu depuis quelques semaines, maintenant que je connais les résultats médicaux de l’autopsie et de la génétique; place à la sérénité et à la foi en l’avenir pour Romuald et Marine. Prête désormais à revivre avec autant d’intensité une vie de mamy (mais je ne mets pas la pression, évidemment !)
LikeLike
Je n’étais pas “pré-câblée” pour devenir grand-mère : les enfants ce n’est pas mon univers de vie, rien à leur dire… Mais Eva, là, ce fut autre chose : l’aimer à distance (1h par semaine pendant 3 mois), lui distribuer des tas de bisous, la promener partout (en poussette, en voiture, en avion, … dans les bras …), la nourrir, la brancher, veiller au bon fonctionnement de ses appareils, faire attention de ne pas arracher sonde ou câbles en se prenant les pieds dedans …etc Une vigilance de tous les instants mais toujours la récompense : elle ne pleurait pas, toujours calme, et ses joues qui appelaient les bisous, et ses bouclettes surgies d’on ne sait où. Lorsque les exercices Padovan déclenchaient tes fous-rires, c’était mon cadeau musical pour la semaine ! Je savais ton retard de développement mental et physique, mais quelle importance ? Depuis ton décès, dans le siège auto à côté de moi, j’ai apprivoisé l’idée de la mort, appris les gestes de 1er secours, découvert l’incroyable énergie déployée par le monde médical pour faciliter ton développement et comprendre tes difficultés, enquêté sur ‘la vie après la vie’, posé un regard nouveau sur la Vie. La naissance d’Eva, sa vie ponctuée de tous ses soubresauts, son décès, tout fut un enrichissement et un bonheur profond, sans questionnement sur le handicap, puisqu’accepté. Notre famille déjà soudée (et les amis) s’est encore plus solidarisée autour d’Eva, elle était le noyau de notre molécule et moi un des petits électrons attentifs et admiratifs (même si parfois ses difficultés à manger agaçaient cela ne durait pas). Merci pitchounette pour tout cela, tu n’es plus là ‘en vrai’ mais tu es là, autour, partout, tout le temps, avec tes ‘signes’ (les arbres, la couleur rouge, les conférences médicales ou philosophiques, ce site BOS, les milliers de photos et vidéos, …). La tristesse a disparu depuis quelques semaines, maintenant que je connais les résultats médicaux de l’autopsie et de la génétique; place à la sérénité et à la foi en l’avenir pour Romuald et Marine.
LikeLiked by 2 people
Je suis triste mais néanmoins admiratif !
Je vous souhaite plein de bonheur pour l’avenir…
Amicalement 🙂
LikeLiked by 1 person
I must get across my passion for your kind-heartedness for those individuals that absolutely need help with in this study. Your personal dedication to passing the message along ended up being certainly helpful and have constantly empowered ladies just like me to attain their goals. Your personal warm and helpful facts can mean so much to me and even further to my colleagues. Best wishes; from all of us.
LikeLike
I really like your writing style, great info , thanks for posting : D.
LikeLike